Drugs administered in medical settings are a robust part of healthcare spending in Minnesota, a new study shows.
Drugs administered in medical settings are a robust part of healthcare spending in Minnesota, a new study shows.
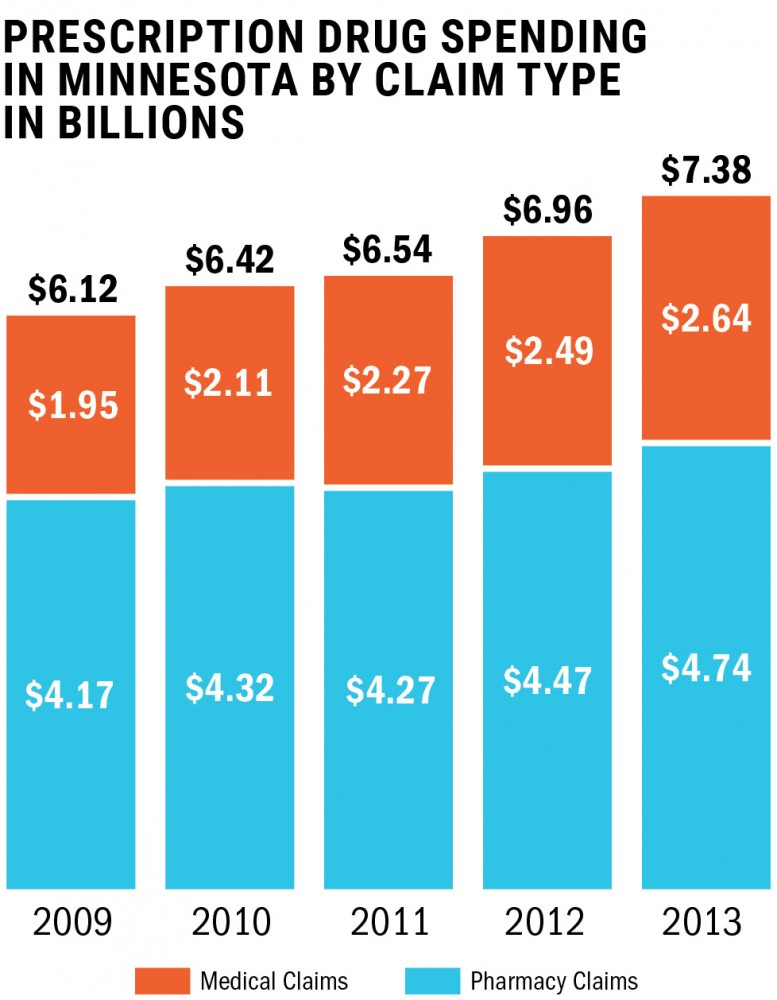
Using data on pharmacy and medical drug sales, researchers from the University of Minnesota’s PRIME Institute and the Minnesota Department of Health (MDH) found that prescription spending rose 20 percent from 2009 to 2013.
The study — released last week — also found the cost-per-claim increased for drugs given to patients in medical settings.
Pharmaceutical claims occur when a patient receives a medical prescription from their doctor and picks it up at a local pharmacy.
Medical claims, however, cover complex drugs that are complicated to use — often those that require injection by a health professional.
Medical drugs are also usually high-cost medications, said PRIME Institute Director Stephen Schondelmeyer.
“Not only are they drugs that are different in some ways, but they’re in a totally different part of your insurance program,” Schondelmeyer said.
The study shows drugs given in medical settings are a bigger piece of Minnesota healthcare spending than previously realized and are growing faster than those on the retail side, Schondelmeyer said.
The data definitively shows that Minnesotans spend about 20 percent of healthcare dollars on drugs. This is more than what they spend on physicians’ services.
Minnesota legislators created the “All Payer Claims” database in 2008 and started collecting data in 2009, he said.
“The database was limited only to state employees and to the Legislature’s use until about a year and a half ago,” Schondelmeyer said.
These databases are often used to look at the prevalence of certain diseases or the total cost of care in states, he said.
Linda Davis, a consultant with the Minnesota Health Action Group, said her expertise is in pharmacy and she acted as a consultant for the study over the past two years.
Many states have all payer claims databases, Davis said, but none have done analyses of medical and retail drug sales like this one.
She said research at MDH is decided by the Legislature, which chooses who researches what and when.
Stefan Gildemeister, director of MDH’s Health Economics Program, also contributed to the study.
“Typically, when we just look at the pharmacy part … it’s much lower than that [spending],” Gildemeister said.
The team also looked at trends, he said, finding that spending in medical settings accounted for over half of the growth in the five years of data.
He said MDH tracks healthcare spending each year, including prescription spending. But in the past, it has only looked at drugs spending in pharmacy settings.
But in 2015, the Legislature made a request for an analysis of the role prescription drugs play in the state’s healthcare system, Schondelmeyer said.
“What we’re missing … is sort of the other part of drug use, which occurs in office settings or is administered in hospitals,” Gildemeister said.
This study is the first in a series of about six total briefs on the data, said Gildemeister, and another set will be published in early 2017.